 Due to the aging of the population, when the degree of systematic determination of prostate-specific antigen (PSA) and rectal ultrasound biopsy of the prostate have become widespread, the physician is faced with an increasing frequency of problems in diagnosing and treating prostate cancer.
Due to the aging of the population, when the degree of systematic determination of prostate-specific antigen (PSA) and rectal ultrasound biopsy of the prostate have become widespread, the physician is faced with an increasing frequency of problems in diagnosing and treating prostate cancer.
In recent years, there has been an increase in the number of diagnosed cases of prostate cancer in the early stages and available for treatment.
Article created Dr. OLEG KORZHYKOV PAVLYUK during moderation Urologist Dr. JOSE ANTONIO QUEIPO
INCIDENCE AND PREVALENCE
Prostate cancer is the fifth leading cause of male tumors of all ages worldwide and in industrialized countries. It is one of the leading causes of death from cancer in the United States and European countries.
It represents 10% causes of cancer death in men. There are predisposing factors. Although the etiology of prostate cancer is unknown, a number of predisposing factors have been implicated in its origin: race, diet, genetics.
Dietary factors have a big influence. Increasing consumption of animal fats has been shown to predispose to the development of prostate cancer factor.
Genetic factors: People with a family history of cancer are two to four times more likely to be at risk. There are undoubtedly hereditary forms of the disease, and the presence of prostate cancer in one or more generations is a risk factor, which can lead to a particularly important observation. Research related to the discovery of genes predisposing to the disease is currently underway.
Prostate cancer is adenocarcinoma, which develops predominantly in the peripheral zone of the prostate (as opposed to the transitional zone, in which adenoma develops). The fact that prostate cancer develops at some distance from the urethra explains the absence of noticeable symptoms in most cases, except in the later stages of the disease.
Prostate adenocarcinoma will develop first inside the gland, and then go beyond the prostate, following the nerve endings and genital tract, after which it deeply invades the seminal vesicles, and finally metastasizes to the deep pelvic muscles and bone structures.
At the histological level, adenocarcinoma develops from a high-grade area of intraepithelial dysplasia, which is considered to be a precancerous condition. As the cancer grows in size, the tumor loses its resemblance to normal prostate tissue.
DIAGNOSTICS
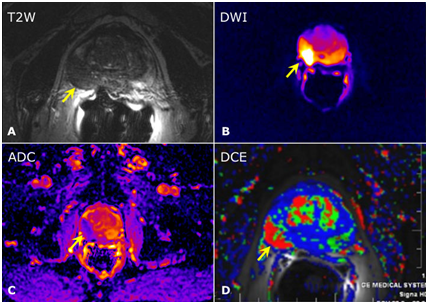
In order to conduct a correct diagnosis for the presence of prostate cancer, it is necessary to answer three questions:
- Should I be screened for prostate cancer?
- When and how to make an early diagnosis?
- Once the diagnosis is made, how to assess the severity of the disease and provide a prognosis for the patient?
Early diagnostic procedures can and should be motivated by only three types of situations:
- Pathological digital rectal examination, regardless of patient age
- Patients presenting with urinary problems
- Patients who want to know exactly the condition of their prostate. In this case, before starting the procedure (physical examination and additional tests), it is necessary to clearly determine which tests are needed and the consequences of their positive result.
HOW TO MAKE EARLY DIAGNOSIS OF PROSTATE CANCER IN SPAIN?
Early diagnosis of prostate cancer is based on digital rectal examination, determination of serum PSA levels and prostate biopsy.
Further research includes Osteoscintigraphy (Nuclear Medicine in Valencia; a radionuclide diagnostic method based on the introduction of a radiopharmaceutical tropic to the bone tissue into the patient's body) to search for metastases and computed tomography.
PROSTATE CANCER TREATMENT IN SPAIN
Valencia offers two treatment options:
- External beam therapy.
- radical prostatectomy.
None of the other types of treatment, such as radium therapy of the prostate, cryotherapy, various types of energy, which are often mentioned in various information sources as an alternative to the two above options, are currently not confirmed, and can only be offered for participation in pilot studies.
EXTERNAL BEAM THERAPY
This high-energy radiation (particle accelerator) at a dose of 65Gy directed at the prostate gland usually includes irradiation of the lymph nodes. It is a treatment that has the advantage of not having to undergo surgery, but the main complications are problems with urination, digestion (proctitis, tenesmus, abdominal cramps), and a significant risk of erection problems with a probability of 40 to 50%. The criterion for the effectiveness of radiotherapy is represented by a decrease in PSA, which at 18 to 24 months after the completion of radiotherapy should be at least below 1 ng and even 0.5ng / ml.
Radical prostatectomy with lymphadenectomy if PSA is greater than 10
This is the removal of the prostate, followed by a ureteral anastomosis. Operative mortality is low (from 0.5 to 1%). Main side effects: temporary urinary incontinence during an adaptation period of 6 to 12 weeks (in exceptional cases there may be permanent urinary incontinence) and, above all, an important change in sexual life (disappearance of ejaculations, erection problems are extremely common, despite the technological operation level). These complications have palliative treatment (implantation of an artificial sphincter for permanent incontinence, minimally invasive treatment of erectile dysfunction with intracavernous injections, tablets). The criterion for the effectiveness of radical prostatectomy is a constant zero level of PSA in the blood.
WHAT TO CHOOSE? SURGERY OR EXTERNAL BEAM THERAPY?
Practice shows that both methods play the same role in terms of effectiveness in the treatment of prostate cancer (patients with prostate cancer are clinically localized with lower PSA up to 15). However, it must be recognized that for patients under 65 years of age, radiation therapy is an undeniable advantage.
Thanks to the author of the article for the information about prostate cancer and its diagnosis and treatment. The material is very useful and relevant.
Based on the article, I would like to ask the question: What predisposing factors influence the development of prostate cancer and what dietary factors can increase the risk of the disease?