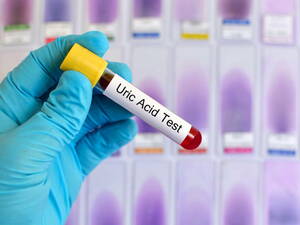
 Treatment for gout is to relieve inflammation and slowly lower uric acid levels. Goutis a well-known and well-studied disease associated with acute inflammation of the joints of the lower and upper extremities of a person, characterized by elevated levels of uric acid, followed by crystallization and precipitation. Hyperuricemia- this is when the concentration of uric acid in serum or plasma exceeds 6.8 mg / dl (approximately 400 micromoles / l). It should be noted that this level of uric acid is its approximate limit when it can crystallize.
Treatment for gout is to relieve inflammation and slowly lower uric acid levels. Goutis a well-known and well-studied disease associated with acute inflammation of the joints of the lower and upper extremities of a person, characterized by elevated levels of uric acid, followed by crystallization and precipitation. Hyperuricemia- this is when the concentration of uric acid in serum or plasma exceeds 6.8 mg / dl (approximately 400 micromoles / l). It should be noted that this level of uric acid is its approximate limit when it can crystallize.
Hyperuricemia (elevated levels of uric acid) is a necessary but not sufficient prerequisite for the development of gout (direct deposition of sodium monourate crystals). Physicians and patients should distinguish hyperuricemia from gout. because most people with hyperuricemia never experience clinical symptomsassociated with the deposition of urate crystals, namely an attack of gout.
Brief description of the disease
The disease itself with its clinical features has been described in the literature for more than two millennia, with its interesting observations and studies. But it wasn't until the second half of the 20th century that evidence emerged that the cause of gout included the deposition of uric acid (sodium monourate) crystals. The key point is the introduction into clinical practice of microscopes using polarized light, which ensured the identification of urate crystals in the synovial fluid of the joints (intra-articular fluid).
Thus, an end was put to the mechanism of this disease and the ambiguous relationship between hyperuricemia and gout was resolved. Further study of this disease has expanded the understanding of the molecular pathophysiology of inflammation in gout, thereby helping to create effective drugs for the treatment of such a common and well-known disease.
Further development of drugs capable of suppressing acute inflammation and eliminating elevated levels of uric acid in the body, provided the opportunity to completely eliminate previously destructive effects in chronic and acute inflammatory processes.
Although modern drugs have had a beneficial effect on the course of gout in most people, nevertheless, this disease remains an urgent problem today, and often with unsatisfactory clinical outcomes, despite successful attempts at treatment. This is very common in poorly trained patients, or in patients who do not follow our guidelines exactly.
What is the treatment for gout? What to take for an acute attack of gout?
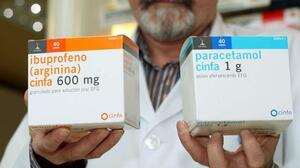 NSAIDs. Non-steroidal anti-inflammatory drugs.
NSAIDs. Non-steroidal anti-inflammatory drugs.
First aid for an acute attack of gout is to prescribe strong oral NSAIDs such as naproxen (500 mg twice a day) or indomethacin (50 mg three times a day), as a good alternative to glucocorticoids for the treatment of a gout flare. It is especially effective for young patients who are less than 60 years of age, without renal or cardiovascular comorbidities or active gastrointestinal diseases.
Non-selective NSAIDs of all types are inexpensive, easy to buy over the counter (some over the counter), and in our experience are as effective and safe as other drugs in treating a gout flare. Other drugs in this class that can be used, for example, ibuprofen (800 mg three times a day), diclofenac (50 mg twice a day), meloxicam (15 mg daily) and celecoxib (200 mg twice a day).
Remember! Do not take more than one NSAID at the same time! Those. You cannot drink Ibuprofen and Diclofenac at the same time, simply because it helps you.
Anti-inflammatory drugs are most effective when treatment is started within the first 48 hours of symptom onset. The dose may be reduced after a significant reduction in symptoms, but the frequency of administration should be maintained for several more days to achieve the optimal anti-inflammatory effect.
Celecoxib, a selective cyclooxygenase (COX)-2 inhibitor, is a very good alternative to ibuprofens, meloxicam, diclofenac (a non-selective NSAID) for gout flares, a single dose of celecoxib at a dose of 200 mg, for no more than two weeks. In practice, we often use 200mg twice a day, which is the maximum dose recommended for rheumatoid arthritis.
Any NSAID (ibuprofen) can be canceled two to three days after the complete disappearance of clinical signs. Typically, the total duration of naproxen therapy for a gout flare is five to seven days. It is likely that the clinical picture will be shorter in patients who are treated within the first 24 hours after the onset of symptoms.
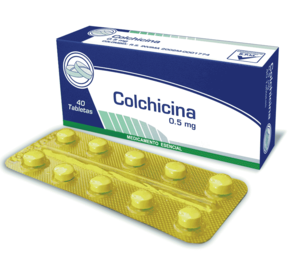 Colchicine / Colchicina / Colchimax / Colchicine
Colchicine / Colchicina / Colchimax / Colchicine
For me, this is an ideal alternative to glucocorticoids (pridnisone) or NSAIDs (ibuprofen) is colchicine, which has actually shown to be effective compared to other drugs when taken within 24 hours of a gout flare. Colchicine should be taken at 1 mg once daily until the outbreak resolves. In some countries, colchicine is available as a 0.5 mg tablet instead of a 0.6 mg tablet. The maximum dose is 2 mg per day according to the new treatment protocols. Previously used up to 6 mg per day, but this is an old regimen, and it is no longer used due to the potential for side effects.
It is worth noting the toxicity of the drug if used improperly. Therefore, before taking it, we recommend that you consult your doctor. The main side effect of colchicine is diarrhea and vomiting. Patients and professionals should pay very close attention to the interaction of colchicine with the following drugs: macrolide antibiotics (azithromycin, clarithromycin, erythromycin), cyclosporine, tacrolimus, amiodarone, quinidine, azole antifungals (ketoconazole), verapamil, CYP3A4 inhibitors (HIV therapy, ritonavir , cobicistat).
Colchicine is a particularly convenient agent for patients already on allopurinol who are in the early phase of a gout flare. Often we meet patients who are familiar with their disease, but have not heard anything about colchicine.
If you have any questions, sign up for a consultation.
Does your lifestyle affect your uric acid levels? Eliminate the following foods from your diet... Find out in this article.
There used to be a so-called demographic profile of gout that fit the "classic" example: a man in his 30s and 60s with gout attacks, who probably also suffers from obesity, hypertension (high blood pressure), and heavy drinking.
But "non-classical" risk groups have emerged, which are becoming more common, and these patient groups are very different from the "classic profile". This includes older patients, organ transplant patients, people taking diuretics, cancer patients, use of drugs such as cyclosporine or tacrolimus (a calcineurin inhibitor), and unfortunately the proportion of women with gout has increased.
What are the clinical manifestations of a gout flare?
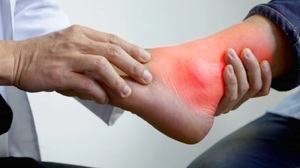 Persistent and elevated levels of uric acid in the body (hyperuricemia) is a common biochemical abnormality resulting from excessive production of uric acid (urate) or when impaired excretion of uric acid kidneys.
Persistent and elevated levels of uric acid in the body (hyperuricemia) is a common biochemical abnormality resulting from excessive production of uric acid (urate) or when impaired excretion of uric acid kidneys.
Therefore, in all patients with gout during their illness, hyperuricemia (saturation of blood serum with urate) is always observed. However, most people with hyperuricemia never experience the clinical manifestations of gout associated with the deposition of urate crystals.
Clinical manifestations of gout include:
- Recurrent flare-ups of inflammatory arthritis (gout flare). Most often in autumn and spring.
- Do you have sharp inflammation of the joint of the finger on the right leg? Read below for what it is.
- This is a strong and acute pain in the joint, redness, the joint "burns", swelling, inability to walk. And usually the patient says that there was no injury! The picture itself usually appears within 12-24 hours, which is quite fast in itself and is typical for this attack. Complete resolution of the earliest outbreaks almost always occurs within a few days to a few weeks, even in untreated people.
- Gout flares are twice as likely to occur during the night and early morning than during the day. Patients often say that they cannot stand on their feet in the morning, because, according to their words, “the knee suddenly became inflamed overnight, while yesterday everything was fine, and I didn’t hit my foot anywhere.”
- Damage to the lower extremities. At least most initial outbreaks affect one joint, most commonly at the base of the big toe (the first metatarsophalangeal joint, known as gout) or the knee.
- Intermittent joint problem, chronic arthropathy.
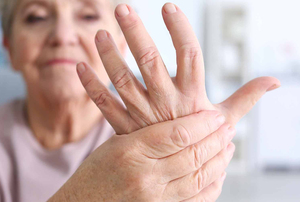 Can gout affect the joints in the fingers and elbows? Yes maybe!
Can gout affect the joints in the fingers and elbows? Yes maybe!
Multi-articular gout flares - A multi-articular pattern is an initial presentation in a small number of patients with gout, but with increasing frequency in subsequent flares. Multi-joint symptoms are especially common in the advanced stages of untreated gout, when multiple recurrences are common. Fingers, elbows, upper jaw.
Signs of inflammation extending beyond the joint are caused by arthritis in several adjacent joints or tenosynovitis. Unusual involvement of the vertebral joints and sacroiliac joints, where gout may occur much less frequently and may cause diagnostic confusion. The most commonly affected area is the lumbar spine. However, most proven cases of gout, manifesting as acute or chronic back pain, have been associated with gastric involvement. There may also be neurological signs and symptoms.
Accumulation of uric acid crystals in the form of external deposits.
Tophi are characteristic accumulations of solid urate, accompanied by chronic inflammatory and often destructive changes in the connective tissue. Tophi are often visible and can be touched and felt (palpated) and may be present on the ears or in soft tissues, including articular structures, tendons, or periarticular bursae. Tofus (tophs) usually do not hurt and are solid in structure. They are visible on the skin, have a slightly yellow or white color. On the ear, they are found in the form of balls, and do not transmit light.
[su_spoiler title="Note to Medical Students and Physicians" style="fancy"]-Chronic inflammation extending beyond one joint with uric acid deposition resembles and is similar to dactylitis seen in other diseases such as psoriatic arthritis, other spondyloarthritis and sarcoidosis. The expansive and destructive changes associated with gouty gout can be mistaken for osteomyelitis and sometimes lead to erroneous amputation of the fingers involved.[/su_spoiler]
 Deposition of uric acid crystals in the kidneys. Nephrolithiasis.
Deposition of uric acid crystals in the kidneys. Nephrolithiasis.
Uric acid stones account for 5 to 10 percent of all kidney stones worldwide; however, they make up 40 percent or more of the stones in areas with hot and dry climates. The most important biochemical risk factor for the development of urolithiasis nephrolithiasis is a persistently low urine pH. And the low volume of urine (with a high concentration of uric acid in the urine) and the acidic pH of the urine promote the conversion of the relatively soluble urate salt into insoluble uric acid.
Patients usually have an attack of renal colic, complain of acute pain in the right or left side. Computed tomography (CT) without contrast/dye usually reveals the presence of a stone. Many patients are advised to confirm the diagnosis with a chemical analysis of the stone. It is worth noting that in conventional radiographs, uric acid stones are transparent and almost impossible to see.
Chronic nephropathy, which in gouty patients most often occurs due to comorbid conditions.
Chronic urate nephropathy is the last stage of chronic kidney disease in chronic gout, caused by the deposition of uric acid crystals in the kidneys (medullary interstitium). The crystals cause a chronic inflammatory response similar to that seen with tophi formation in other parts of the body, which eventually leads to interstitial fibrosis and chronic kidney disease.
The clinical stages of the disease ("Gout flares", "Recurrent gout flares", "Chronic gout") occur sequentially, with a corresponding clinical severity that often coincides with the frequency of gout flares. Therefore, treatment with uric acid-lowering (antihyperuricemic) drugs is deterrent, and provides effective recovery for the patient if urate saturation does not rise above <6 mg/dl or 357 micromoles/l.[su_divider]
High level of uric acid. How and with what drugs to control a chronic disease. Where to begin?
Heavy drinking and alkalinization of the urine (potassium citrate) can cause clear uric acid stones to dissolve. Either potassium citrate or potassium bicarbonate can be taken with a typical dose of 30 to 80 mEq/day. This regimen can dissolve already existing pure uric acid stones and prevent new stones from forming.
For us, alkalization of urine with potassium citrate salts is currently the most preferred, as sodium loading with sodium citrate or sodium bicarbonate may increase calcium excretion and contribute to the formation of calcium stones in some patients. Alkalinization is carried out so that the pH of the urine is between 6.5 and 7. We also recommend that patients drink enough liquid so that the volume of urine within 24 hours is at least two liters.
Many patients are familiar with Allopurinol and Probenecid ("Probalan", a uricosuric agent). These are well-known, proven and old drugs that have proven themselves well and have demonstrated their effectiveness.
If uric acid kidney stones cannot be prevented despite alkalinization of the urine (or who cannot tolerate additional alkali) and higher fluid intake, we recommend treatment with a xanthine oxidase inhibitor (Allopurinol). These patients usually have hyperuricosuria (greater than 1000 mg/day [6 mmol/day]), but xanthine oxidase inhibitors are warranted even in patients with recurrent stones and lower levels of urinary uric acid excretion.
 Allopurinol / Allopurinol / Zyloric
Allopurinol / Allopurinol / Zyloric
It is worth noting that Allopurinol is used for patients with elevated uric acid when there is no acute attack of gout. Otherwise, the effect will be the opposite.
This is a truly time-tested product. Very popular among patients, often used in clinical practice for chronic uric acid control, easy dosage and availability.
From clinical practice, patients often turn to us when a gout attack has already manifested itself. People, without knowing it and through no fault of their own, begin to take allopurinol, after which the attack worsens even more. This drug is very effective in preventing seizures when taken on a continuous basis, even when there are no prerequisites for an aggravation of the clinical picture.
Febuxostat / Febuxostat / Adenuric / Uloric
One of the newest and most effective drugs for controlling uric acid levels. Replaced allopurinol. Indeed, it is used in clinical practice, where allopurinol is not effective enough. Febuxostat is actively replacing allopurinol, but in February 2019, the Food and Drug Administration (FDA) issued a warning about the increased risk of death from Uloric (febuxostat) compared to allopurinol.
This conclusion is based on a detailed review of the results of clinical safety trials of the drug, during which an increased risk of death from cardiovascular diseases, from all causes, was found with the use of Uloric. Patients with gout and established cardiovascular disease who received febuxostat had a higher rate of death from cardiovascular disease compared with patients who received allopurinol.
A new warning about this risk is now being added to the Uloric/Adenuric prescribing information (including the boxed warning). Today, new guidance limits the previously approved use of Febuxostat to patients. Febuxostat should only be prescribed to patients who have an inadequate response to the maximum dose of allopurinol, who cannot tolerate allopurinol, or for whom treatment with allopurinol is not recommended, and who do not have cardiovascular disease.
Probenecid / "Probalan" / Probenecid
Reduces the reabsorption of uric acid in the renal tubules, thereby increasing its excretion, reducing the deposition of urates. But to date, the main therapeutic indication for the use of probenecid is to support the level of penicillinemia in the treatment of diseases.
Probenecid reduces the excretion of penicillins by increasing and prolonging the plasma levels of penicillin, ampicillin, methacillin, oxacillin, cloxacillin, or nafcillin.
It also serves to prevent renal toxicity during chemotherapy with cisplatin. In the treatment of syphilis, it maintains an effective level of antibiotics. The use of this drug in conjunction with colchicine is useful in an acute attack of gout. However, it is strictly contraindicated in patients with hepatic and renal insufficiency.
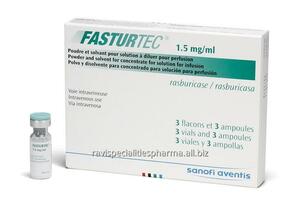 Rasburicase / Rasburicase / Elitek/Fasturtec/
Rasburicase / Rasburicase / Elitek/Fasturtec/
The drug is exclusively used intravenously to control the level of uric acid in oncology, it is released only for hospital use. Requires strict dosing. High probability of side effects, up to an anaphylactic reaction. Therefore, this application is strictly regulated.
This drug is interesting for very high levels of uric acid in the body, which is not even associated with metabolism, but with massive cell destruction. This is when chemotherapy is used to destroy the tumor, and when the cancer cells are destroyed, their toxic contents are released into the human body.
By the way, one of the basic principles of the use of chemotherapy is that you cannot immediately destroy one kilogram of cancer cells, because the body simply will not survive such a toxic release of their destruction.
Glucocorticoids / Glucocorticoids.
We now rarely use oral glucocorticoids (prednisone, prednisolone), especially in situations where the patient is not a candidate for intra-articular corticoid injections. There are many patients who have contraindications to the use of non-steroidal anti-inflammatory drugs (ibuprofen, naproxen), in which case we can prescribe corticoids for them.
The starting dose of prednisone or prednisolone is 30 to 40 mg per day. The dose is reduced gradually. The duration of therapy depends on several factors (before taking, consult your doctor). Drugs in this class have a fair amount of side effects, so we strongly recommend that you do not self-medicate unless you suddenly want to become a diabetic, for example.























One thought on “Лечение подагры. Лечение острого приступа. Мочевая кислота.”
Sincerely,
I would like to express my deep gratitude to the author of the article for the information on the treatment of gout. The material was presented very clearly and understandably, which greatly helped me understand the essence of this disease.
Based on the article, I had a question about how hyperuricemia leads to the development of gout. What exact mechanisms and processes occur in the body when the level of uric acid exceeds the limit and crystallization occurs? Are there ways to prevent or slow down this process?
I would appreciate your clarification on these issues.
Sincerely, Igor